Essential Tools in Modern ETT Kits
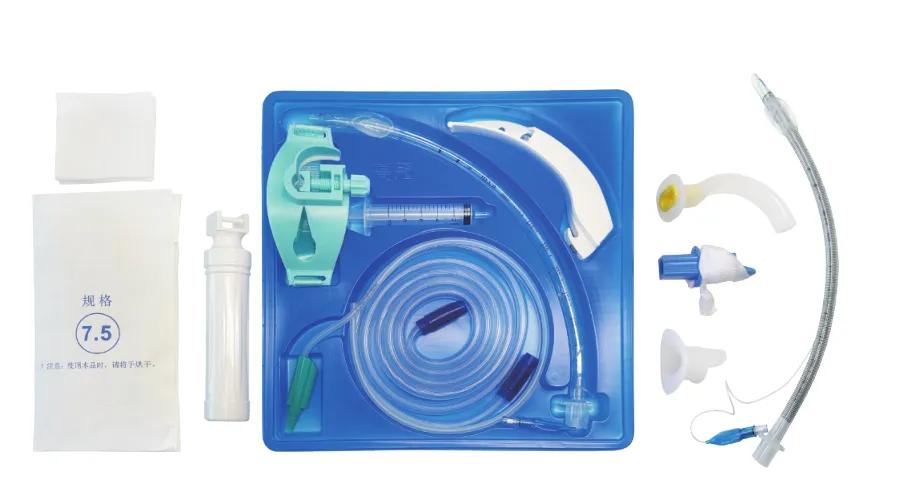
Endotracheal tube kits, often abbreviated as ETT kits, comprise several essential tools fundamental to successful intubation procedures. Key instruments include laryngoscopes, intubation tubes, and suction devices. Each tool plays a critical role in ensuring smooth, efficient, and safe airway management. Let's explore these further:
Laryngoscopes
These devices are indispensable for aiding the visualization of a patient's vocal cords during intubation. Traditionally equipped with blades and handles, modern versions now incorporate LED lights, significantly improving visibility in dimly lit environments and contributing to safer intubation practices.
Intubation Tubes
These tubes are designed to maintain an open airway in patients under anesthesia or those unable to breathe independently. The tube's function is pivotal as it facilitates direct access to the patient's trachea, ensuring oxygen delivery and ventilation.
Suction Devices
Employed to clear the airway of obstructions, suction devices are crucial for preventing complications such as aspiration and ensuring an unobstructed pathway for intubation.
Continual advancements in technology have ushered enhancements like ergonomic designs and material improvements, allowing healthcare professionals to perform intubation with increased precision and care. These innovations ensure that clinicians can adapt to various scenarios while maintaining patient safety as a primary objective.
Understanding Tube Sizes and Cuff Designs
Endotracheal tubes come in various sizes, tailored to accommodate patients of different ages and anatomical structures. Understanding these variations is crucial for healthcare providers to ensure appropriate airway management.
Tube Sizes
Pediatric patients require smaller tubes compared to adults, highlighting the importance of size selection based on the patientâs age and physical characteristics. This customization is essential to prevent trauma and maximize efficiency during procedures.
Cuff Designs
The cuffs attached to endotracheal tubes are really important for keeping the tube properly positioned inside the trachea and stopping stuff from getting into the lungs accidentally. These high volume but low pressure cuffs work by spreading out the force across the airway wall, so they don't damage the tissue as much during long procedures. On the flip side, there are those smaller volume cuffs that create higher pressure seals. They tend to form a better barrier against leaks, though doctors usually only reach for them when absolutely needed because of the increased risk factor involved. Most modern practices favor the gentler approach unless specific circumstances demand otherwise.
More and more research points to high volume low pressure cuffs being the best choice overall. These cuffs seem to work really well at preventing airway injuries while also helping patients recover better after intubation procedures. Looking at various studies about managing airways, we see they actually cut down on problems like damage to the mucosa lining and risk of aspiration. This makes them pretty valuable tools in today's hospitals and clinics where doctors are always looking for ways to improve care without adding extra risks.
Preparing for Quick Intubation: Best Practices
Patient Positioning and Airway Assessment
Getting ready for an intubation really begins with how we place the patient and checking out their airway first. The so-called sniffing position matters a lot because when done right, it lines up the mouth, throat area, and voice box, giving better access during the procedure. To achieve this, most clinicians will lift the patient's head just a bit while extending their neck forward. Simple things work wonders here too – regular hospital pillows often do the trick just fine, though there are specialized tools available for airway management if needed. Sometimes nurses get creative with whatever they have on hand to make sure everything goes smoothly.
Getting the patient properly situated comes first before moving on to airway evaluation. When assessing the airway, clinicians need to look out for things that might make intubation tricky. Think about those big tonsils or someone with a small jaw that makes visualization difficult. The Mallampati score system works really well here. It basically looks at what parts of the mouth can be seen when the patient opens their mouth and sticks out their tongue. This gives a pretty good idea of how hard the actual intubation will be. Most experienced providers find these standardized checks extremely helpful. They don't just make things safer, they actually give medical staff more confidence going into the procedure. Fewer surprises mean better outcomes for everyone involved.
Equipment Readiness and Sterilization Protocols
Getting equipment ready and making sure everything stays sterile isn't just important for intubation it's absolutely essential. Before starting, medical staff need to go through their pre-intubation checklist carefully. They check if they have all the right stuff on hand like laryngoscopes, those flexible endotracheal tubes, and working suction devices. Sometimes hospitals even keep backup equipment nearby just in case. Taking this extra time upfront really pays off because it stops those frustrating moments when something goes missing or breaks during the procedure. Clean, functional tools mean fewer interruptions and better outcomes for patients undergoing intubation.
Sterilization protocols matter just as much as having all the right equipment ready to go. When it comes to cleaning reusable tools, most facilities rely on either autoclaving or chemical disinfectants these days. Both methods work pretty well at cutting down on infection chances. Hospitals have seen some scary numbers when staff skip proper cleaning steps though. One study showed that hospitals with lax sterilization practices had infection rates almost double those places where they followed strict guidelines. Keeping things clean isn't just about following rules either. Patients actually recover better when their surroundings are free from harmful microbes, and doctors get fewer complaints about postoperative complications too. So yeah, taking sterilization seriously really does pay off in multiple ways.
Techniques for Efficient Intubation Using ETT Kits
Direct Laryngoscopy vs. Video-Assisted Approaches
Healthcare workers regularly argue about whether to stick with old school direct laryngoscopy or go with newer video-assisted methods for putting tubes in patients' throats. Direct laryngoscopy was what everyone used back in the day, giving doctors a straight view at those vocal cords. But there are problems too, especially when things get tough during intubation. This can mean longer times getting the tube in place and sometimes even trouble accessing the airway properly. Video laryngoscopes change the game though. They give better views from different angles with proper lighting, making it easier to get that tube where it needs to go, particularly in complicated situations. Studies show doctors succeed on their first try more often with video scopes in tricky cases, which explains why they're becoming so popular for managing hard airways. According to guidelines from the American Society of Anesthesiologists, video assisted techniques should be首选 for difficult cases because of all these advantages. Still, many practitioners find regular direct laryngoscopy works just fine for everyday procedures since it doesn't require fancy gadgets and is pretty straightforward to use.
Securing the Tube Post-Insertion
After inserting an endotracheal tube (ETT), keeping it secure becomes absolutely essential for both patient safety and proper breathing support. There are several ways to do this: adhesive tape works well for many patients, though some facilities prefer specialized fixation devices or even stitches in critical situations where extra stability is needed. The goal is simple really – keep the tube from moving around during normal patient activity, transfers between units, or any medical procedures. Regular checks are a must too. Healthcare workers should look at the tube's position visually and confirm its function through capnography readings. We've all seen what happens when tubes get displaced during transport or when patients shift positions unexpectedly. That's why most experts strongly recommend investing in good quality tube holders with adjustable features. These tools help prevent those dangerous situations where the tube slips out or gets blocked, making them worth every penny for hospitals trying to reduce complications from improper ETT placement.
Common Pitfalls in Rapid Intubation and How to Avoid Them
Overlooking Patient Positioning Under Stress
During emergencies, the intense pressure often causes medical staff to miss what should be a basic step patient positioning before intubation. When this happens, things get really complicated fast because visibility drops and getting into the airway becomes much harder, which raises chances of failing the whole procedure. Medical journals back this up too many reports show how bad positioning leads directly to problems like low blood pressure and trouble breathing properly. I remember hearing about a real case from a coworker who worked in the ICU. They had someone lying flat on a regular hospital mattress and kept trying to intubate without success several times. The solution? Stick to those positioning guidelines no matter how chaotic things get. We've found that having specific checklists designed for emergency situations works wonders. These lists help remind everyone involved about critical steps that need doing even when time is running out and stress levels are through the roof.
Device Selection Errors and Time Management
Getting the right intubation device matters a lot for preventing problems and making the whole process go smoother. When doctors pick the wrong gear, things tend to fall apart pretty quickly, putting patients at greater risk than necessary. Clinical data shows failure rates jump significantly when the wrong tools get used, so this really needs attention. Take one case we saw recently with video laryngoscopy equipment - someone actually got injured because nobody checked if they had the proper setup beforehand. Time management plays a huge role here too. Good practices start with looking over all the equipment ahead of time, doing regular practice runs, and getting everything ready properly for surgery. All these steps help speed things up while keeping accuracy high, which cuts down on bad outcomes. From our experience, teams that spend extra time planning and practicing tend to have much better results during those critical moments in the operating room.
Case Study: Lessons from Real-World Scenarios
ICU Intubation Complications Analyzed
Intubation in the ICU comes with its share of problems, including things like pneumothorax and when tubes end up in the wrong place (esophagus instead of trachea). These issues really worry medical staff because they put patients in serious danger. Research indicates that about 10 to 15 out of every 100 people get a collapsed lung from the procedure while in intensive care units. Looking at real cases shows why these mistakes happen so often. Sometimes doctors make errors during the process or just don't follow all the rules properly. Take poor visibility during insertion for example. This usually happens when someone hasn't had enough hands-on experience or gets distracted under pressure. When this occurs, the tube goes down the wrong pipe entirely. What we learn from these situations points clearly toward one solution: ongoing education and strict following of established protocols remains essential if we want to keep complications to a minimum.
To address all these challenges, healthcare professionals have created various guidelines aimed at making things safer during ICU intubations. Many experts now suggest using ultrasound guidance when possible because it helps doctors see exactly where they're placing tubes inside patients' airways. This approach cuts down on the chance of causing a collapsed lung and makes sure the breathing tube ends up in the right spot. Simulation training has also become really important lately. Doctors and nurses practice on mannequins that mimic real emergencies so they can get better at handling high-pressure situations without risking actual patients. These kinds of protocols aren't just theoretical either they make a real difference in saving lives across hospitals everywhere.
Key Takeaways for Emergency Situations
Getting good at emergency intubation means following protocols built from real world cases and experiences. The main points are quick evaluation of the situation, picking the right tools for the job, and acting fast to get that airway secured before things go south. Before jumping in, doctors need to check their gear and run through what they'll do next so they're ready when the moment comes. Most experts recommend sticking to an intubation checklist religiously and doing practice runs regularly to keep skills sharp under pressure. These preparation steps really help clinicians stay calm in high stress situations and ultimately save lives when every second counts in critical care settings.
Medical experts keep pointing out how following set emergency protocols really boosts chances of successful intubations. The National Emergency Airway Registry put together some pretty telling numbers showing hospitals that stick closely to these guidelines tend to have fewer complications and more successful procedures down the line. Looking at actual hospital data makes it clear why standardized methods matter so much for saving lives during emergencies. Regular training sessions combined with protocol adherence form the backbone of good outcomes. When doctors and nurses actually implement what they learn from these studies on a daily basis, they're far better equipped to handle those high-stakes situations where every second counts during an intubation attempt.
FAQ Section
What are endotracheal tube kits?
Endotracheal tube kits, abbreviated as ETT kits, include several key components such as laryngoscopes, intubation tubes, and suction devices, essential for intubation procedures to ensure efficient airway management.
Why is tube size important in intubation?
Tube sizes are crucial because they must be appropriately tailored to the patient's age and anatomical structure to prevent trauma and enhance efficiency during intubation.
How do cuffs on endotracheal tubes function?
Cuffs are designed to secure the tube within the trachea and prevent aspiration. They come in various designs, like high-volume, low-pressure, to minimize airway injury during intubation.
What is the purpose of video-assisted intubation?
Video-assisted intubation offers enhanced visualization, especially in complex cases, improving angles and lighting for more accurate and successful intubation.
How can intubation complications be reduced in ICU settings?
Reducing complications involves following standardized guidelines, incorporating advanced imaging techniques, and simulation-based training to ensure accuracy and preparedness during intubation processes.

